
The Mount Sinai Adolescent Health Center (MSAHC) provides free, comprehensive, integrated, confidential health care to young people ages 10 to 26.
We have 32,000 patients in our patient roster and provide services to more than 12,000 of them each year. Most of our patients are low income and 90% of them are youth of color. They come from communities that are negatively impacted by the social determinants of health with resulting disparities and inequities. These are the families most negatively impacted by the COVID-19 pandemic.
The great majority of our patients are uninsured and MSAHC makes all health care services accessible at no cost, pays for all necessary laboratory tests and medications, and provides MetroCards to patients. This approach is necessary to remove barriers to desperately needed health care during ordinary times but is essential during the pandemic.
Patient Numbers During the COVID-19 Pandemic
New York State’s stay-at-home orders went into effect the evening of March 22. From March 23 to June 30 we served a total of 3,462 patients who made 6,077 visits.
- From March 23 to March 31 we served 430 patients. In primary care, 203 patients made 246 in-person medical visits and 3 in-person emergency dental visits. 227 patients made 296 mental health telehealth visits.
- From April 1 to April 30 we served 880 patients. In primary care, 524 patients made 745 in-person medical visits and 9 emergency dental visits. 356 patients made 1,239 telehealth mental health visits.
- From May 1 to May 31 we served 1,080 patients. In primary care, 693 patients made 1,032 in-person medical visits and 9 emergency dental visits. 387 patients made 1,307 telehealth mental health visits.
- From June 1 to June 30 we served 1,459 patients. In primary care, 984 patients made 1,449 in-person medical visits and 40 dental visits. 475 patients made 1,297 telehealth mental health visits.
Providing Critical in-Person Care
The MSAHC did not close during the COVID crisis. We remained open Monday through Saturday 8:30 am to 6:00 pm to provide necessary care to young people. While during the pandemic we encouraged young people to stay home and only come in for health care that couldn’t wait, young people came to the clinic with a number of immediate health needs. Some patients were concerned about possible symptoms of coronavirus or requested coronavirus testing. Others came for additional medical problems including a variety of illnesses, from upper respiratory symptoms to abdominal complaints. We have been able to see and reassure patients while keeping them from going to already overwhelmed Emergency Departments at Mount Sinai and elsewhere. Attending to their needs now rather than later also prevents patients from needing to be admitted to the inpatient unit later due to delayed treatment. By remaining open we have been able to see patients with a goal of minimizing the use of other hospital resources.
In addition, when young people present to the clinic with an emergent need, we provide not only medical services, but also health education, mental health services and emergency dental services on site daily as needed.
Now that NYC is opening, we continue to provide in person services Monday through Saturday. The MSAHC has resumed appointments for routine primary care, immunization updates, and sick care. The appointments have been staggered and structured to abide with social distancing mandates. We have also worked on a practice re-design to create new work flows allowing patients to arrive and be seen in the most efficient and effective manner. The MSAHC continues with our overnight and Sunday phone coverage, and we provide inpatient care for our patients in the event of hospitalization at Mount Sinai.
The Need for Supportive Spaces
With schools closed and no after-school services or sports programs, young people need a place where their emergent needs can be addressed, their questions can be answered and they feel seen and supported in these times of unpredictability, stress and tremendous need. Many places that provide health care and other crucial services to young people are closed. Patients have greatly appreciated that we are open. We are seeing new patients who usually receive services at other sites in NYC that are no longer open to in-person services. In response to this need, the MSAHC decided to increase the upper age limit for patients from 24 years old to 26 years old.
Unsure where to turn, some adults in the community are coming to us, requesting help with health insurance enrollment, seeking advice on what to do, and asking about where to get services. We have been helping any person who shows up in these times of need.
New Approach in Services due to COVID-19
Virtually overnight, the COVID-19 pandemic reached crisis levels in New York City and created a new set of challenges and opportunities for the MSAHC as we navigated how to provide sexual and reproductive health care and other essential services to vulnerable adolescents and young adults while protecting patients and staff from illness. The sudden shift in our patient care paradigm, scheduling and overall operations has been a major challenge but also a great testament to our commitment to accessible, compassionate and confidential care for those in need.
Staff and patient safety remains our number one priority. We screen patients for COVID-19 symptoms as soon as they come through the door, and put them in isolation as indicated. The medical staff wear personal protective equipment (PPE) to screen and to see the patients with symptoms consistent with COVID-19. Once the patient receives services, they are handed needed medications onsite and immediately sent home.
Many patients are already wearing masks and gloves when they arrive at the MSAHC. If they are not, we give them masks, instruct them on how to wear them, and provide information on why face coverings and social distancing are important. In the clinic, social distancing protocols are followed among the patients, among the staff and between patients and staff.
Staffing has been staggered into “teams” to allow onsite care while minimizing the risk of possible exposure from coworkers. Staff have been willing and committed to continue to work in this model.
Increased Telehealth Services
To minimize face-to-face encounters, we have made a number of service adjustments. MSAHC physicians are on call every night and Sunday to support patients. We have added telehealth services to provide care to patients who do not need to be seen in person. Telehealth services now include nutrition counseling, health education, mental health services and prenatal services.
Since >70% of our patients have active MyChart (the patient portal of our electronic medical record) accounts, we used this tool to mass message patients about our availability and send updates on COVID-19 and other health issues. We also encouraged providers to use MyChart to screen and advise patients accordingly in a secure environment. We continue to have an unprecedented use of MyChart and Telephonic Encounters.
Sexual and Reproductive Health Care
Many of the visits during the pandemic have been for sexual and reproductive health, including family planning: Depo-Provera; Long Acting Reversible Contraceptives (LARC) and LARC on demand; other contraceptives and emergency contraceptives; pregnancy testing; prenatal care; STI testing and treatment; HIV testing and treatment; PrEP and PEP to prevent HIV; transgender health care; and abnormal laboratory test follow up. The NYS DOH designated sexual and reproductive health services as “essential services” during the COVID-19 pandemic.
While working remotely many of our staff are reaching out to patients who are due for contraceptive refills to ensure that they do not run out while schools and other medical providers are closed.
Prenatal and Teen Parenting Services
Prenatal services are provided in person or via telehealth for trimester-specific health education and other prenatal services as appropriate. To make this possible, we provided all prenatal patients with blood pressure cuffs and taught them how to take and track their own blood pressure. In keeping with our goal to promote education, a sense of community and support among our patients and their partners, we implemented virtual prenatal care groups adapted from the Centering Pregnancy model and have given access to e-learning childbirth education courses to our patients who are in the third trimester of pregnancy. Young parents also use our teen parenting services for their children’s health care. These include infants delivered during the pandemic.
Response to Young People’s Increased Need for Mental Health Services
During this period of social isolation, young people’s need for support is even higher than usual. Mental health staff remain in the clinic to provide care to young people who come to the MSAHC for other services and need mental health care for depression, anxiety and other mental health needs.
In addition to in-person mental health services, our mental health staff are providing ongoing psychiatric services and psychotherapy from home via telehealth and telephone. Mental health clinicians using telehealth provide the full range of services they provide in face-to-face sessions. These include but are not limited to psychosocial assessments, treatment planning, safety planning, victim support services, personal advocacy, and more.
We anticipate that young people in New York will be dealing with the impact of COVID-19 for an extended period. The virus has traumatically disrupted their lives. Young people face the disappointment of cancelled graduations, family celebrations and other plans, stress from financial uncertainty, and grief over the loss of loved ones and friends. We expect symptoms of anxiety, post-traumatic stress disorder, depression, suicidality and other mental health conditions to increase.
To address these needs, there has been updated training and supervision on Trauma Focused Cognitive Behavior Therapy for all mental health staff. We are also providing additional virtual group therapy and support group services, including two new Dialectical Behavior Therapy (DBT) groups. These groups are designed to support adolescents who have difficulties with emotional dysregulation. We are in the process of creating new virtual support groups focused on bereavement and grief, as 33% of patients who completed a survey reported that they had lost a loved one. Our relationships support group for young women, transgender support group, and HIV positive support group have continued to meet virtually.
Patient Engagement
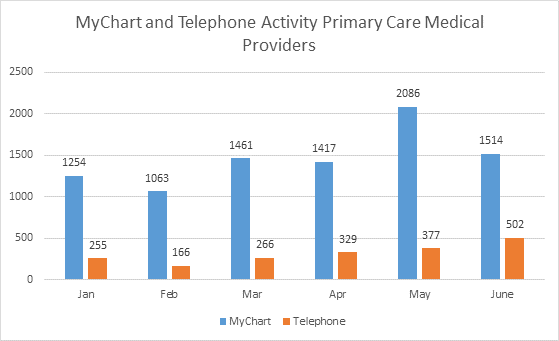
Our patients continue to have full access to providers and other staff in person; via our Health Squad app, which includes the ability to text; by telephone; and via MyChart (the patient portal of our electronic medical record). We are virtually engaging patients at higher numbers. When we compare MyChart and telephonic activity in February 2020 to March 2020, there was a 40% increase in MyChart communications and a 60% increase in telephonic encounters. From March through June, MyChart communications increased by 70% and phone communications doubled. MyChart remains an essential and well-utilized tool for individual communications and blast informational messaging.
Our Legal Services’ COVID-19 Response
As part of our medical-legal partnership with Youth Represent (YR), the legal advocates and lawyers have provided legal services remotely. Since mid-March, our legal service has provided 61 pieces of legal counsel, worked on 16 cases, reviewed Record of Arrests and Prosecutions (RAP) sheets for eight clients, provided five pieces of legal information, and referred seven young people to outside resources. There has been a significant uptick in use of legal services. From April 22 to June 30, the legal team served 36 young people providing 46 services.
Peer Education (SPEEK) Program and MSAHC Mapping Project
Our peer education program Sinai Peers Empowering Education through Knowledge (SPEEK) has continued meeting regularly using online video conferencing platforms. SPEEK is a multifaceted program that includes a peer education training program, evidence-based health education workshops and services for local middle schools, high schools and community based organizations.
In response to COVID-19, SPEEK adapted its education and outreach activities so they could be done virtually. SPEEK…
- Worked with community partners to conduct virtual sexual and reproductive health education on social media platforms.
- Created collaborative content for Instagram to highlight youth views and experiences related to healthy relationships, consent, body image, mental health and more.
- Is developing a community youth outreach project to engage young people in health and wellness practices and link them to MSAHC services.
- Will host virtual peer trainings on a variety of sexual and reproductive health topics.
- Adapted its summer mapping program with MAPSCorps to be conducted virtually. Peer educators will use phone calls and online research to create resource guides for their assigned neighborhoods.
- Begun collaborating with the Arnhold Institute for Global Health to create and disseminate graphics to educate young people on issues related to COVID-19.
In addition, an MSAHC social worker has regularly facilitated discussions during SPEEK meetings to provide on-going support to our peer educators during this uncertain time. Based on feedback from the peer educators, they appreciate the space that has been provided for them to process their feeling related to COVID-19 and racial injustice.
In addition to the initiatives described above, we continue to provide critical support to young people while prioritizing patient and staff safety in the following ways:
- Some staff are working remotely. To support this transition, we have distributed 29 additional iPhones and other devices; set up Skype Business for all 125 staff members to facilitate communications among staff; obtained 30 licenses for 90 days from GoToMeeting for staff meetings; activated Medisprout to support telehealth video visits with individual patients as well as group therapy sessions; and plan to purchase 3 licenses for Zoom to support remote trainings, all-staff meetings and more.
- A small team of sexual assault prevention staff, including our YES Program Coordinator, co-led an effort to create a crowdsourced COVID Victim Services Resource Guidefor providers and is currently making an accessible resource guide for NYC-based survivors/victims. Our YES Program is also planning a virtual, interactive rape crisis counseling training for staff.
- We put together and continue to update this resource list, which includes resources related to access to food, financial assistance, mental health, and more. It is also available in Spanish. We have shared the resource list on social media, and sent it out to patients via MyChart and our Health Squad app.
- We have developed a COVID-19 self-care & mental health guide on our website, which has been sent to patients via MyChart and continues to be promoted on social media.
- The social work staff have produced a wellness guide for young people. This guide will also provide content for a series of social media pieces for maintaining mental health and well-being during this crisis. Other products such as a resource guide are also being completed.
- We are planning a “Not Alone” video campaign giving young people and staff a platform to share their personal experiences with COVID-19 and let young people impacted by the virus know that they are not alone.
- We put together a sexual health Instagram Live series to virtually answer young people’s questions about a variety of sexual health topics.
- We continue to use social media to provide young people and families with useful and relevant health and wellness information, and to keep them up to date about the MSAHC during this time.
Financial Impact
While we provide services at no cost to patients, we do accept health insurance, mostly Medicaid. Because we have seen a decrease in patient volume due to the coronavirus crisis, we are losing income we would have received from these insured patients. In addition to this loss of income, we face additional expenses as we prioritize patient and staff safety, establish telehealth services and expand phone access. For these reasons, we anticipate running a $2.5 million deficit in 2020.
Some of the additional expenses include:
- Surgical Face Masks
- Procedure Masks
- N95 Masks
- Isolation Gowns
- Patient Gowns
- Face Shields
- Shoe covers
- CoronavirusTesting kits
- Sanitizing (Clorox) Wipes
- Hand Sanitizers
- Personal Protective Equipment Kits
- “No Touch” Thermometers for Patient Screening at the door
- Rolling stands to take vital sign equipment from room to room rather than moving the patients
- Additional signage to instruct patients about new policies during the COVID-19 outbreak
- Technology for working from home (as described above), including to provide telehealth and telephonic psychotherapy
- iPads and iPhones for staff to work remotely
- We also continue to do multiple deep cleanings of the clinic and constantly disinfect clinic areas as appropriate.
- Blood pressure machines for pregnant patients
About the Mount Sinai Adolescent Health Center
The MSAHC was established in 1968. From modest beginnings, it has grown into a nationally and internationally-recognized, comprehensive, integrated health center that serves young people ages 10-26 and any children they may have. Our population includes young people from some of the most vulnerable communities in NYC, including youth in foster care and those aging out of foster care, immigrants, homeless youth, LGBTQ youth and many other groups. Services are developmentally appropriate, confidential and provided at no cost to patients. The services we provide include services for patients with eating disorders, youth who use alcohol and other substances, youth with mental health conditions including bipolar disorder, schizophrenia, anxiety, post-traumatic stress disorder, depression and suicidality as well as youth with learning disabilities including dyslexia and other processing and attention issues. Our program has an emphasis on wellness and prevention and in helping all adolescents flourish and fulfill the promise of adolescence. The program is built on the principles of positive youth development, social justice and achieving equity.
Since 2010, the MSAHC has been designated at the highest level (Level 3) Adolescent Health Patient-Centered Medical Home by the National Coalition for Quality Assurance. Young people hear about us from their peers, are referred by parents, other family members, their school or community-based organizations, or they find out about us through our website, app, blogs and social media. They come here not just because we are accessible, but because they know they will be welcomed and respected.
MSAHC opened its first school-based health center (SBHC) in 1982 and today has school-based health centers in six high school buildings, serving 24 high schools and middle schools. This allows us to meet young people where they are.
Young people come to our Center from all five boroughs of New York City, other areas of New York State and from as far as New Jersey, Pennsylvania, and Washington, DC. All are seen regardless of their insurance status or ability to pay, and at no cost to them.
Our mission is to break down economic and social barriers to health care and wellness for young people by providing vital services—high-quality, comprehensive, confidential and free—for all who come to us. And we advance adolescent health as a national imperative by serving as a leading center of clinical care, specialized training and innovative research.
Young people need to be physically and emotionally healthy to make it in this world. High-quality care is their right—and our responsibility.


